
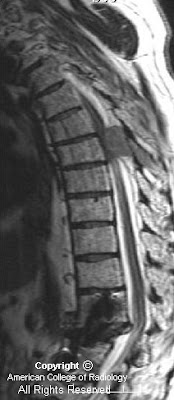

Findings
Sagittal T1-image (Figure 1) in a patient with multiple myeloma shows a large epidural mass in the midthoracic region with associated cord deformity. The mass displaces the epidural fat. Postsurgical changes are seen in the lower spine consistent with repair of a prior compression deformity. Marrow signal is heterogeneous throughout.
Sagittal T2 image (Figure 2) in a patient with multiple myeloma shows a large epidural mass in the mid-thoracic region with associated cord deformity. The normal CSF signal is completely displaced by the mass. Post-surgical changes are seen in the lower spine consistent with repair of a prior compression deformity. Marrow signal is heterogeneous throughout
Post-contrast T1 axial image (Figure 3) demonstrates compression of the cord anteriorly by a large epidural mass.
Diagnosis: Myeloma with cord compression
Myeloma patients with abnormal neurological findings suggesting cord compression should be evaluated by MRI when available. Imaging exam should be primarily targeted, based on the results of motor and reflex tests, rather than pain or sensory level.
Spinal cord compression is a neurological emergency that may be diagnosed by the presence of a mass lesion abutting the cord with cord deformity, or abnormal cord T2-signal.
Acute spinal cord compression is a potentially devastating neurological emergency that requires both prompt diagnosis and intervention to prevent permanent impairment. The frequency of metastatic cord compression is increasing as cancer prevalence rises and new treatment modalities prolong patient survival. Close cooperation between clinical services and diagnostic radiologists is essential for patient triage. This is especially true in cases where patients cannot be fully examined neurologically. Magnetic resonance imaging is the study of choice in evaluating these patients; it is noninvasive, does not involve radiation, and provides for investigation of both osseous and soft tissue lesions.
Many etiologies can result in acute spinal cord compression. These include trauma, infection, neoplasm, degenerative disc disease, and others. Differentiation between these various causes of acute cord compression relies on a combination of clinical history, neurological exam, and imaging findings. However, the constellation of imaging findings indicative of cord compression are similar, regardless of the causative process.
In evaluating the patient, close cooperation between clinical staff and the diagnostic radiologist is essential. Information from the neurological exam is critical for localization of the lesion and optimization of the imaging protocol. Whole spine imaging is generally undesirable as it is more time-consuming, expensive, and difficult for patients who are often in considerable pain. It further lowers resolution on exams that are often suboptimal, secondary to severe patient pain and patient movement. Spinal sensory levels on neurological examination may be up to several segments below the anatomic level of cord compression. Evaluation of motor function and reflexes is very useful for lesion localization.
There has been considerable debate within the literature on the precise radiological definition of cord compression. Animal models suggest that both direct mass effect on the cord and impingement on the epidural venous plexus contribute to pathology. Spinal cord compression may be defined as the presence of a mass lesion abutting the cord with the complete loss of intervening CSF. This must be accompanied by deformation of the spinal cord, or the presence of signal changes within the cord. The findings are best visualized on T2-weighted images. If the patient is concurrently symptomatic, acute intervention is mandated with the specific type of intervention determined by the underlying disease process.
Nessun commento:
Posta un commento