

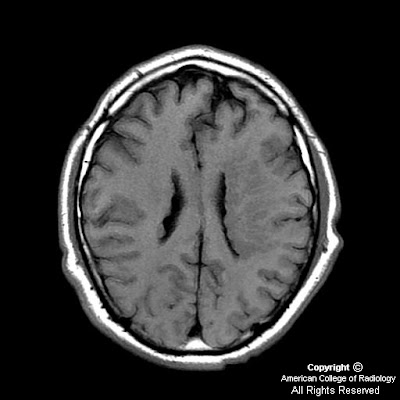



Findings
Figure 1 and Figure 2: Increased density in the periventricular region. This is consistent with subependymal gray matter.
T1 axial (Figure 3), T1 sagittal FLAIR (Figure 6), and T2 coronal FSE (Figure 4) images demonstrate isointensity to normal gray matter on all sequences. T1 post-gad image (Figure 5) shows no abnormal enhancement.
Differential diagnois:
- Subependymal (periventricular) heterotopia
- Subepedymoma
- Hamartoma (tuberous sclerosis)
- Subependymal hemorrhage
- Vascular malformation
Diagnosis: Subependymal (periventricular) heterotopia
Heterotopia, simply defined, means a collection of neurons in an abnormal location, due to an arrest in migration.
There are three clinically useful classifications of gray matter heterotopia:
- subependymal heterotopia
- band heterotopia
- subcortical heterotopia
Subependymal, which is the most common of the three, tends to present with epilepsy in the second decade of life. Subcortical and band heterotopia tend to present with epilepsy earlier in life (first decade). Additional brain anomalies may also be associated.
Initial imaging modality is typically CT in a postepileptic patient. Findings include increased density in a periventricular distribution without enhancement or calcification. Proper window settings are essential for proper diagnosis. Low level and window allow for greatest contrast. All three are most easily diagnosed with MRI, which demonstrates isointensity to normal gray matter on all sequences without postgadolinium enhancement.
Subependymal heterotopia (SEH) can occur in isolation or with other neurologic and metabolic disorders.
Anatomically, it is subdivided into three subtypes
- unilateral focal
- bilateral focal
- bilateral diffuse.
All types typically present with epilepsy in the second decade of life with disorders of cognition being proportionate to the area of heterotopia. MRI shows small areas of gray matter, which is isointense to mature gray matter, protruding into the ventricular lumen. X-linked causes have been found in many of the bilateral diffuse cases, resulting in more dramatic neurodevelopmental disorders in males. The same causative gene mutation has been associated with Ehlers-Danlos syndrome.
Band heterotopia is diagnosed by visualization on MRI of a smooth layer of gray matter separated from the cortex and ventricles by white matter. This may also be called “double cortex.” Neurodevelopmental disability is proportionate to the thickness of the heterotopic “band.” The manifestations of this x-linked disease are more drastic than SEH; males suffer from lissencephaly, while females suffer from band heterotopia. Clinically, females typically present with epilepsy in the first decade of life.
Subcortical heterotopia is anatomically classified into two forms
- nodular form
- curvilinear form.
Much less is known about this classification of heterotopia than the others mentioned. Patients present with varying degrees of mental and motor delay and epilepsy in the first decade of life. Imaging shows various sizes of clusters of improperly migrated neurons throughout the white matter. Many theories regarding the cause of this subtype are currently being studied.
Nessun commento:
Posta un commento