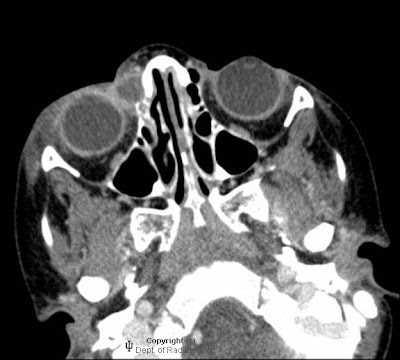
Findings
FindingsCT: There is marked dilation of the superior sagittal sinus with low attenuating density, containing high density septations. The expansion and density extends into the straight sinus. There is a large peripherally calcified lesion at the right aspect of the dilated superior sagittal sinus near the torcular Herophili. There is also severe hydrocephalus, with involvement of the third and lateral ventricles.
MRI: There is a heterogeneous lesion expanding the superior sagittal sinus and torcula, demonstrate mostly hyperintense signal on T1 and T2, containing multiple septations, with suggestion of fluid/fluid level, without definite contrast enhancement. There is extension into an enlarged vein of Galen. There is a area of low signal on the right side corresponding to calcification seen on CT.
No central flow is demonstrated in the posterior portion of the superior sagittal sinus, corresponding to the lesion.
Angiography (images not shown): Showed mass-effect in the posterior parietal-occipital regions without filling by contrast. No evidence of tumoral blush, AV shunting, or aneurysm.
Follow-up CT: Showed significant decrease in mixed density material expending the superior sagittal sinus from the vertex to the torcula, consistent with interval resorption of clot.
Differential diagnosis for the neonatal studies:
- Dermoid
- Vascular tumor
- Congenital variant
- Giant dural sinus thrombosis
Diagnosis: Dural sinus thrombosis, with involvement of the superior sagittal sinus, straight sinus, and vein of galenDiagnosis confirmed on the subsequent CT, which demonstrated partial resorption of thrombus.
DiscussionDural sinus thrombosis represents formation of clot in the dural sinus
Clot spreads from dural sinus to cortical veins, resulting in hemorrhage and infarct
Will progress to infarction in approximately 50%
Clinical presentation:
- Presenting symptoms include headache, focal neurologic deficits, papilledema
- Numerous etiologies, such as hypercoagulable state, infection, inflammation
- Dehydration and infection is a common cause in children
- Idiopathic in 10 to 30% of cases
- No particular age or sex predilection
- Morbidity and mortality from progression to venous infarction
- Treatment include thrombolysis
Imaging:
- Early findings are subtle
- Classic sign is the "empty delta" seen on contrasted imaging
- Thrombus seen in dural sinus and cortical veins
- Sinus is occluded and expands
- Appearance depends on age of clot
- Vessels may recanalize
CT:
- "Empty delta" sign represents non enhancing thrombus in the dural sinus with surrounding enhancing dura in contrast enhanced CT
- "Cord sign" is hyperdense dural sinus clot seen in non contrasted CT
- May see associated hemorrhage or edema
MRI:
- Signal on T1 and T2 depends on age of thrombus
- On GRE, the thrombus may "bloom," depending on stage of hemorrhage
- On MRV, there is absence of flow
Angiography:
- Thrombosed sinus does not fill