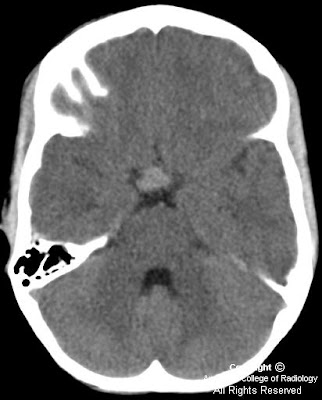
Findings
Initial head CT without contrast: Subarachnoid hemorrhage seen filling the quadrigeminal cistern, suprasellar cistern, and surrounding sulci. This is most prominent in the posterior fossa. There is associated intraventricular hemorrhage and moderate obstructive hydrocephalus. CT head angiography: There is a 3mm L superior cerebellar artery aneurysm
Diagnosis: Subarachnoid hemorrhage secondary to rupture of left superior cerebellar artery aneurysm.
The most common presenting symptom of SAH is "the worst headache of my life." The peak incidence is around 40-60 years of age and is slightly more common in females. Subarachnoid hemorrhage localized to the posterior fossa is uncommon in the setting of trauma and suggests posterior circulation aneurysmal rupture. Hemorrhage is most extensive at the site of aneurysm. Most common sites of aneurysm are in order of decreasing frequency: Anterior communicating artery, posterior communicating artery, middle cerebral artery, anterior cerebral artery, basilar artery, internal carotid artery, PICA, vertebral artery, and superior cerebellar artery. Saccular, berry, or congenital aneurysms constitute 90% of all cerebral aneurysms and are located at the major branch points of large arteries. Infectious or mycotic aneurysms are situated peripherally and comprise 0.5% of all cerebral aneurysms. Amyloid angiopathy typically produces more peripheral areas of hemorrhage.
Staging, grading or classification criteria
Grading:
- Grade 1: Thin SAH = 5 mm
- Grade 2: Thick SAH > 5 mm
- Grade 3: Thin SAH with mass lesion(s)
- Grade 4: Thick SAH with mass lesion(s)
Lower grades have better admission Glasgow coma scores & discharge Glasgow outcome scale scores.
Clinical Course
50% mortality, 15% rebleed within first 24 hr
Natural history: Breakdown & resorption from CSF
Complications: Acute hydrocephalus, delayed hydrocephalus, vasospasm
Acute hydrocephalus
- Rare; usually obstruction of aqueduct or 4th ventricular outlet by clotted SAH
bstructive, non-communicating hydrocephalus
- Asymmetric ventricular dilatation
Delayed hydrocephalus
- Arachnoid granulation defect in CSF resorption
- Obstructive communicating hydrocephalus
+ Symmetric ventricular dilatation
Vasospasm
- May develop quickly (2-3 days post-injury)
- Peaks 7-10 days post-injury, threat remains up to 2 weeks
- Uncommon cause of post-traumatic infarct
Radiologic overview
Best diagnostic clue: Hyperdense CSF on non-contrast CT
Suprasellar, basal, Sylvian & interhemispheric cisterns most common location
Hemorrhage most extensive at site of aneurysm
CT without contrast: 95% positive in first 24 hr, < 50% by 1 week
CTA 90-95% positive if aneurysm = 2 mm
FLAIR: Hyper intense; FLAIR more sensitive than CT but less specific
MRA: 85-95% sensitive: Insufficient detail for surgery
Difficult to see on T1WI, T2WI & GRE
T1WI: CSF mildly hyper intense ("dirty")
Angiography: Negative in 15% of aSAH; repeat positive < 5%