Findings
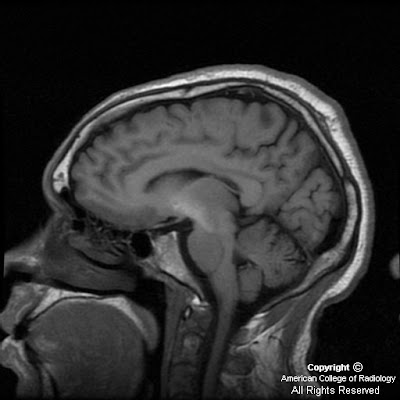
FindingsFigure 1: The panorex demonstrates a displaced fracture of the right mandibular ramus near the angle, as well as a fracture line through the left parasymphseal mandibular body, through an incidental partially calcified mass.
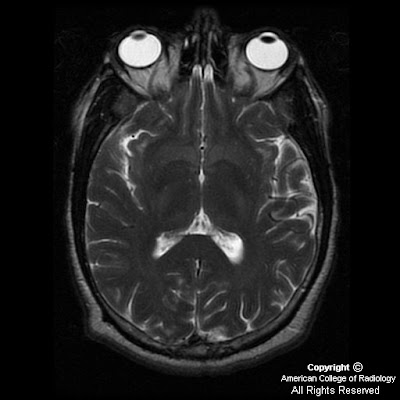
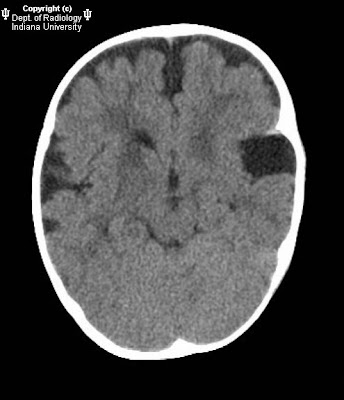
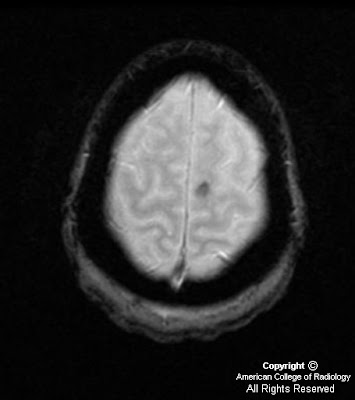
Figure 2, Figure 3, and Figure 4: Axial, coronal, and sagittal CT images demonstrate a collection of radio-opaque tooth-like structures surrounded by a thin radiolucent peripheral rim. In addition, there are associated unerupted teeth.
Differential diagnosis for calcified masses in the mandible:
- Calcifying odontogenic cyst (Gorlin’s cyst)
- Calcifying epithelial odontogenic tumor (Pindborg tumor)
- Cementoma
- Fibrous dysplasia
- Foreign body
- Odontoma
- Ossifying fibroma
- Osteoma
- Synovial osteochondromatosis
- Focal sclerosing osteomyelitis
- Chondrosarcoma
- Osteosarcoma
- Metastasis
Diagnosis: Pathologic fracture of the left mandibular body through a compound odontoma and a fracture of the right mandibular ramusEmbyrologically, the dental lamina proliferates along the future dental arches. At intervals beneath the lamina, tooth buds are formed, each composed of an enamel organ, a dental papilla, and a dental sac.
The enamel organ differentiates to include ameloblasts, which elaborate enamel in response to the production of dentin by odontoblasts within the underlying dental papilla. The dental sac forms both a layer of cementum around the dentin that covers the root, as well as the periodontal ligament, which attaches the cementum to the surrounding bone.
Odontogenic cysts and tumors are derived from the enamel of the tooth crown, epithelial remnants from the root sheath or dental lamina, or from the tooth germ itself (the enamel organ, dental papilla, and dental sac). Symptoms, when present, may be related to tooth devitalization, secondary infection, absence of teeth due to impaction or lack of development of the normal tooth, convergence of crowns due to a mass growing between the roots of two teeth, or expansion of the mandible or maxilla itself.
Generally asymptomatic except for their association with unerupted teeth, odontomas are the most common type of odontogenic tumors. They represent a hamartomatous growth of ameloblasts and odontoblasts, which abnormally elaborate enamel and dentin within the mass. Compound odontomas are generally located in the anterior jaw and by definition contain denticles, structures within the mass with the macro- and microscopic appearance of small teeth. In contrast, complex odontomas are generally found in the molar regions of the jaw and contain disorganized dental tissue. Complex odontomas require histopathologic analysis to differentiate them from other lesions.
Odontomas generally undergo surgical enucleation due to malpositioning and impaction of adjacent teeth. In addition, the epithelial components can give rise to a dentigerous cyst. The lesion does not recur after excision.