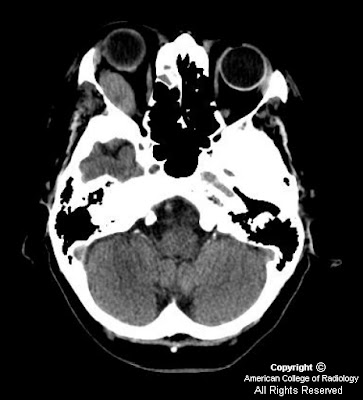



Findings
Figure 1: Axial section from a non-contrast head CT at the level of the orbits shows an oval-shaped soft tissue mass involving the right lateral rectus muscle consistent with an extramedullary plasmocytoma.
Figure 3, Figure 4, and Figure 5: There are bifrontal lytic bone lesions with soft tissue components consistent with plasmacytomas as well as additional lytic lesions in the calvarium.
Single AP view of the CXR (not showed) shows a Mediport in place. There are multiple old rib fractures as well as an old fracture of the right clavicle.
Diagnosis: Multiple myeloma with extramedullary plasmacytomas
Multiple myeloma is characterized by malignant single clone of plasma cells with a wide spectrum of manifestations. The malignant clone of plasma cells secretes malignant paraprotein (heavy and/or light chain immunoglobulin) which in turn leads to a variety of clinical consequences. The peak incidence of multiple myeloma is between 50-60 years of age. The pathophysiology of myeloma is diverse. Over proliferation of plasma cells may hinder production of normal marrow elements resulting in anemia, thrombocytopenia and leukopenia. There is impaired humoral immunity secondary to an inadequate complement of antibodies. Overproduction of clonal antibodies leads to hyperviscosity, amyloidosis and renal failure. Plasma cell proliferation may result in soft tissue tumors (plasmacytomas) or lytic lesions within bone producing pain, pathologic fractures and hypercalcemia.
The diagnosis of multiple myeloma rests on three clinical criteria: (1) M-protein in the serum and/or urine. Electrophoresis of the serum and/or urine reveals increased monoclonal immunoglobulin in the blood or light chains in the urine. Paraprotein levels directly correlate to tumor burden (2) Clonal bone marrow plasma cells or plasmacytoma (3) Related organ or tissue impairment (hypercalcemia, renal insufficiency, anemia, or lytic bone lesions). Myeloma may have a variety of presentations in the skeleton: a permeative pattern, purely lytic lesions (as seen in this case), or as a bubbly lytic lesion i.e. medullary plasmacytoma. Because the solitary bony lesions of myeloma are purely lytic, they may not be conspicuous on bone scan. Skeletal lesions in myeloma involve the hematopoetic axial skeleton i.e. skull, spine and pelvis.
Plasmacytomas are masses of clonal plasma cells involving the bone (medullary) or soft tissue (extramedullary). These entities can be found independent of myeloma, however, medullary plasmacytomas progress to myeloma in 50-60% of patients while the extramedullary variety progresses to myeloma in 11-30% of patients. Plasmacytomas may precede clinical evidence of myeloma by 3-5 years. Medullary plasmacytomas arise from the bone marrow. The most common presentation of medullary plasmacytomas is pain related to bony destruction. Medullary plasmacytomas may present as solitary lytic lesions with a narrow zone of transition on plain radiographs. Rarely, they present as a lucent lesion of bone resembling aneurysmal bone cyst or giant cell tumor. Sclerotic appearing plasmacytomas are associated with POEMS syndrome (polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy and skin changes). On magnetic resonance imaging, medullary plasmacytomas are low in signal on T1 and high in signal on T2 weighted-images.
Extramedullary plasmacytomas arise from submucosal plasma cells. Eighty percent of extramedullary plasmacytomas occur in the head and neck. Involvement of the nasophayrnx and paranasal sinuses is common with most symptoms related to tumor size and location. Extramedullary plasmacytomas appear as nonspecific soft tissue density on imaging studies. Because of submucosal growth, deep biopsy, open biopsy or excision is necessary for histopathologic examination. Other clinical features of myeloma must be excluded before making the diagnosis of solitary extramedullary plasmacytoma. There are three clinical stages of extramedullary plasmacytoma. Stage I is local disease. Stage II disease is characterized by regional lymph node spread or bony erosion. Stage III represents disseminated disease (including bony metastases) which carries a better prognosis then multiple myeloma. Primary treatment of symptomatic plasmacytomas is radiotherapy. Recurrence is common for which additional treatment with surgery or chemotherapy may be considered.
Nessun commento:
Posta un commento