
Findings
Figure 1: Contrast enhanced T1 weighted image of the sella demonstrate normal enhancement of the pituitary gland with a small round hypoenhancing focus consistent with microadenoma which fills in on later sequences.
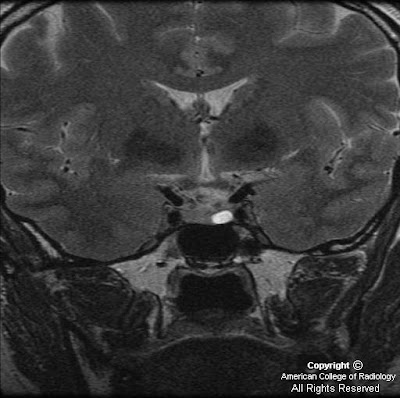
Figure 2: Coronal thin section T2 weighted image demonstrates a bright focus on the left side of the pituitary gland, in the region of previously noted hypoenhancement, consistent with a microadenoma.
Diagnosis: Pituitary microadenoma
Pituitary microadenomas account for 10-15% of all intracranial tumors, though most are found incidentally during autopsy. Pituitary microadenomas are usually benign and slow-growing. Most are asymptomatic. There is 10-20% prevalence in the general population. Prolactin-secreting adenomas or prolactinomas are the most common type, accounting for 30-40% of symptomatic microadenomas. One percent of microadenomas are multiple.
The typical presentation of prolactinoma is a young female with primary or secondary amenorrhea and infertility, with associated galactorrhea. Though usually seen in females, prolactinomas can occur in males with delayed puberty or primary hypogonadism. Growth hormone secreting adenomas, another type of pituitary microadenoma, present with acromegaly in adults and gigantism in adolescents. Prolactinomas typically occur in the 25-30 year age group, while growth hormone-secreting adenomas occur between 30-50 years of age.
Pituitary microadenoma is an intrapituitary lesion surrounded by cresecentic rim of compressed anterior pituitary. Though predominately located within the sella turcica they rarely can have an ectopic origin within the sphenoid or cavernous sinus, pituitary stalk, or third ventricle. By definition, microadenomas are less than 10 mm in diameter. The differential for pituitary microadenoma includes non-neoplastic cysts, such as Rathke cleft cyst and pars intermedia cyst; craniopharyngioma; and pituitary hyperplasia.
On imaging studies, the microadenoma is classically well-circumscribed and enhances less than surrounding normal gland. Microadenomas are isodense to normal pituitary and cannot be seen on non-contrast enhanced CT if uncomplicated by hemorrhage or cyst. On dynamic contrast-enhanced CT, two-thirds of pituitary microadenomas typically appear as hypodense masses surrounded by normally enhancing pituitary. On MR, non-contrast T1 and T2 weighted images may not show microadenomas as they appear isointense to the adjacent pituitary. Dynamic contrast-enhanced MR is the diagnostic imaging modality of choice because microadenomas enhance more slowly than normal pituitary. With contrast-enhanced MR, 70-90% of lesions appear as a relatively hypoenhancing lesion surrounded by enhancing pituitary. Scans should be obtained at 10-15 second intervals following rapid bolus injection of contrast. It is important to to note that 10-30% of microadenomas are only seen on dynamic contrast enhanced MR imaging.
Conservative treatment is recommended for “incidentalomas,” including clinical and imaging follow-up, unless there is a change in size in which case ophthalmological and endocrinological evaluation is recommended. For functioning microadenomas, medical therapy, such as bromocriptine and dopamine agonists, i.e. cabergoline, may reduce prolactin secretion to normal in 80% of cases. Surgical treatment is curative in 60-90% of cases.
Nessun commento:
Posta un commento