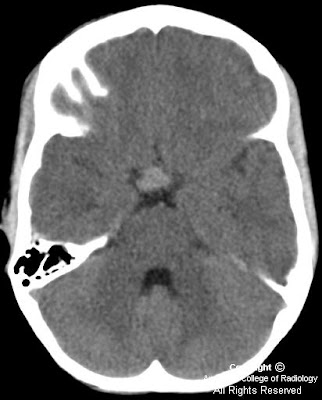



Findings
Figure 1 (unenhanced CT): Well-circumscribed, noncalcified, hyperdense mass in the suprasellar cystern (arrow).
Figure 2 (MRI T1 w/o contrast): Sellar/suprasellar mass, isointense to white matter, with mass effect on the undersurface of the optic chiasm, without hydrocephalus.
Figure 3 (Coronal T1 w/contrast): Mass demonstrates homogenous enhancement.
Figure 4 (Sagittal T1 w/contrast): Extension of mass along a thickened pituitary stalk into the hypothalamus.
Diagnosis: Granulomatous hypophysitis
Granulomatous hypophysitis is a rare inflammatory process, accounting for approximately 1% of pituitary lesions. This entity may be mistaken for a pituitary neoplasm, such as an adenoma. Unlike lymphocytic hypophysitis, which predominantly affects females, young women in late pregnancy or postpartum period, granulomatous hypophysitis appears to have no gender predilection and average age at diagnosis is greater than 40 years.
Patients often present with a headache. Other symptoms may include hypopituitarism, diabetes insipidus, hyperprolactinemia, or symptoms associated with chiasmal compression. While preoperative diagnosis is desirable, diagnosis is most often made postoperatively. Granulomatous hypophysitis may be idiopathic or associated with systemic granulomatous disease, such as tuberculosis, syphilis, sarcoidosis, Crohn’s disease or Wegener’s granulomatosis. It also may be associated with foreign body reactions, such as a ruptured Rathke’s cleft cyst or mucocoele.
Imaging characteristics demonstrate a sellar mass with a tongue-like suprasellar extension. The lesion may contact or infiltrate the basal hypothalamus. Pituitary stalk thickening is often a prominent feature. The lesion usually shows marked, homogenous enhancement, although heterogeneous and ring-like enhancement also occur.
Nessun commento:
Posta un commento