



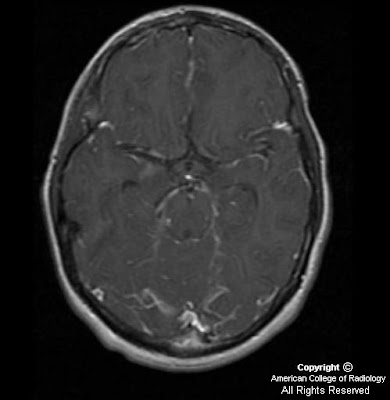
Findings
On T1-weighted images, foci of hyperintense signal are identified within the bilateral amygdala.
Axial T1-weighted image demonstrates abnormal high signal in the region of the right amygdala.
Axial T1 image demonstrates a focus of high signal in the medial aspect of the right temporal lobe.
On axial T2-weighted images the lesions are not well seen.
There is no enhancement present on the axial T1-weighted fat saturated image with contrast
Diagnosis: Neurocutaneous melanosis
Neurocutaneous melanosis is a rare form of a congenital, nonfamilial neuroectodermal dysplasia in children, who may demonstrate intracranial symptomatology, usually within the first decade of life. It has been identified in patients with von Recklinghausen’s disease and Sturge-Weber disease. The congenital skin lesions may occur as multiple or giant hairy pigmented cutaneous nevi.
The leptomeningeal involvement is suspected by demonstration of melanocytosis in cerebrospinal fluid and confirmed by the biopsy of the brain or spinal cord.
Melanocytes occur normally in the CNS, most commonly in the pia mater covering the cerebral and cerebellar hemispheres, anterior surface of the brainstem, basal surface of the brain and anterior surface of the spinal cord. Benign leptomeningeal melanosis occurs when there are areas of proliferation of sheets or nests of melanocytes without frank malignant change. Malignant leptomeningeal melanosis occurs when there is brain and/or spinal cord invasion or the melanocytes demonstrate malignant changes. Leptomeningeal melanosis is malignant in 40-50% of patients with neurocutaneous melanosis.
Parenchymal involvement is demonstrated as hyperintense signal on non-contrast T1-weighted MR images. The free radicals within melanin are paramagnetic, thus producing T1 and T2 shortening. Lesions generally appear hypointense on T2WI. Parenchymal lesions generally do not enhance on contrast enhanced T1-weighted images, while leptomeningeal lesions usually demonstrate marked enhancement.
Patients commonly present with signs and symptoms related to hydrocephalus. Treatment is palliative, with no significant alteration in the course of the disease.
Nessun commento:
Posta un commento