



Findings
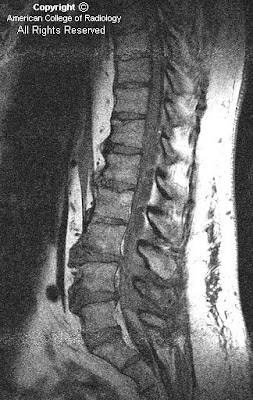
Sagittal T1 (Figure 1), T2 (Figure 2) & T2 with fat sat (Figure 3) images reveal an extradural multilobulated cystic structure which extends from the level of the T11 to L3 vertebrae. This is causing mass effect on the thecal sac. Post contrast, there was no enhancement.
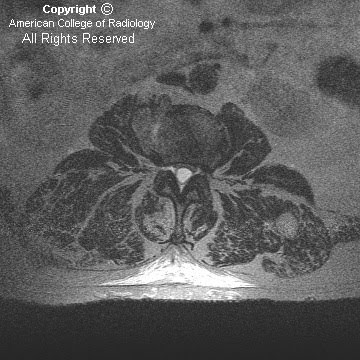
Axial T2 images (Figure 4, Figure 5, and Figure 6) once again reveal an extradural cystic structure which is causing mass effect on the thecal sac. No nerve roots are contained within the cystic structure.
Diagnosis: Spinal extradural meningeal cyst
Spinal meningeal cysts are uncommon, representing only 1-3% of all spinal masses. The pathogenesis of meningeal cysts is still unknown. Histologically, the lining of the cyst cavity may or may not be shown to be arachnoidal tissue, therefore the terms extradural arachnoid cyst and extradural meningeal cyst are used interchangeably.
Spinal meningeal cysts occur most frequently within the thoracic spine (66%), followed by the lumbar and lumbosacral spine (12%), thoracolumbar spine (12%), sacral spine (6.6%) and the cervical spine (3.3%). Most of the lesions are located posteriorly in the spinal canal. Thoracic located cysts most commonly occur in adolescents whereas sacral cysts are more commonly found in adults.
Spinal cysts mostly present through nerve compression symptoms which can be intermittent or slowly progressive. Intermittent exacerbation can occur with postural changes and Valsalva maneuvers.
MR imaging is extremely helpful in demonstrating an extradural cystic structure with CSF signal intensity. MRI can also help in identifying displacement of epidural fat and subarachnoid space, inclusion of nerve rootlets and extension into intervertebral foramina. Once the cyst is identified, CT myelography can be utilized to demonstrate a connection between the cyst and the subarachnoid space.
A classification system termed the Nabors Classification has been developed for meningeal cysts:
- Type I: lesions are extradural meningeal cysts without spinal nerve root fibers, which can be subdivided into
Type 1A extradural meningeal cysts
Type 1B sacral meningoceles
- Type II meningeal cysts are extradural and contain nerve root fibers (Tarlov’s perineural cyst)
- Type III meningeal cysts includes all intradural arachnoid cysts
Differential diagnosis for extradural arachnoid cysts include
- Intradural arachnoid cysts
- Neurenteric cysts
- Perineural cysts
- Synovial cysts
- Meningocele
- Cystic neoplasm
- Congenital and traumatic dermoid
- Inflammatory cysts or cysticercosis
Asymptomatic patients with meningeal cysts can be followed by imaging. Surgery is the treatment of choice for symptomatic patients. Immediate pain relief post surgery is common, but recurrent back pain is frequently encountered at long-term follow-up.
Nessun commento:
Posta un commento