



Findings
Figure 1: Prenatal ultrasound demonstrates a 4 x 5 cm intracranial lesion in the region of the right middle cranial fossa, with multiple cystic and heterogeneously echoic soft tissue areas.
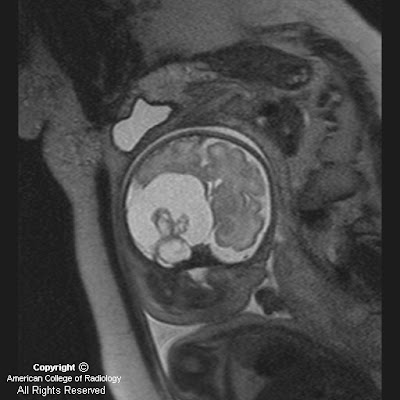
Figure 2, Figure 3, and Figure 4: MR images at 32 weeks 3 days gestation. Coronal (Figure 2) and sagittal (Figure 3) single shot T2 weighted (SShT2) images and axial (Figure 4) fast field echo (FFE) image of the fetal head show a large cystic lesion with multiple internal cysts and soft tissue components in its inferior aspect in the region of the right temporal lobe. (SShT2: repetition time 15000 milliseconds, echo time 120 milliseconds, flip angle 90, number of excitations 2)
(FFE: repetition time 5.3 milliseconds, echo time 2.6 milliseconds, flip angle 60, number of excitations 2)
Figure 5: Newborn non-enhanced axial CT image shows a multicystic heterogeneous lesion within the right temporal lobe containing calcification.
Differential diagnosis of complex cystic neonatal intracranial masses:
- Teratoma
- Astrocytoma
- Hemangioma
- Cystic ependymoma
Diagnosis: Congenital cystic intracranial neoplasm
Congenital brain tumors represent only 0.5-1.9% of all pediatric brain tumors, but of these, intracranial teratomas are the most common tumor in the neonatal period. They are congenital neoplasms derived from all three embryonic layers and contain ectodermal, endodermal, and mesodermal elements and are thought to arise from embryonic cells that fail to differentiate or migrate. They originate in the 3rd to 4th weeks of fetal development, have mixed density, and are most commonly found in the pineal and suprasellar regions.
Extragonadal teratomas are thought to arise from misplaced, pluripotential, primordial germ cells. According to one theory, some of the embryonic germ cells fail to migrate normally and these ectopic germ cells become embedded in or near midline structures. The ectopic cells retain their pluripotent capabilities and may develop into teratomas or other types of germ cell neoplasms.
Intracranial teratomas can be divided into two categories with those occurring in the cerebral hemispheres and those occurring in the pineal region. Those appearing in the cerebral hemispheres are typically large and are usually discovered in the newborn period. Those in the pineal region manifest symptoms later on and are usually smaller. Intracranial teratomas are extremely rare tumors and are usually diagnosed after birth, but they have been discovered prenatally via ultrasound.
Of the intracranial prenatal neoplasms, teratomas and primitive neuroectodermal tumors (PNETs) are the most common. If a heterogeneous prenatal cystic mass is identified, a congenital cystic teratoma should be at the top of the differential diagnosis. Imaging features of teratomas show both lipid and calcification. Characteristics that help to differentiate teratomas from PNETs are the presence of lipid and the lack of blood breakdown products, which are often seen in PNETs.
When ultrasound demonstrates a brain lesion, prenatal MRI can be used to define the characteristics and extent of the tumor while also delineating the relationship of the lesion with adjacent structures. MRI is not only useful for correct diagnosis, but it also may obviate the need for immediate postnatal imaging of the newborn and findings can determine potential resectability and guide surgical planning. In this case, the prenatal MR imaging was used in prenatal diagnosis and aided in pregnancy and surgical management. While it has been shown that a fetus with an arachnoid cyst can safely undergo normal spontaneous vaginal delivery, the diagnosis of teratoma in this patient altered both the method and timing of delivery in this patient.
Nessun commento:
Posta un commento