


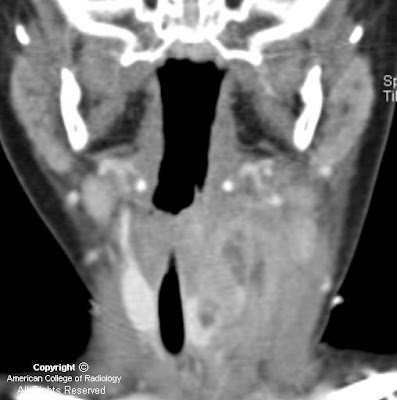
Findings
Figure 1: Neck CT, contrast enhanced, at level of pyriform sinus. The left pyriform sinus is effaced by an inflammatory mass.
Figure 2: Neck CT, contrast enhanced, at level of subglottic trachea. The image demonstrates continuation of the large inflammatory mass with small areas of necrosis or abscesses. Note displacement of the trachea to the right and lateral displacement of the carotid sheath vessels. Reactive lymphadenopathy is present in the internal jugular chain.
Figure 3: Neck CT, contrast enhanced, at level of the thyroid gland. The image shows a mixed attenuation mass in the enlarged left lobe of the thyroid. This mass arises from extention of the extrinsic anterior and lateral inflammatory mass with phlegmon and abscesses from an infected 4th branchial apparatus cyst.
Figure 4: Neck CT coronal reformation, contrast enhanced. There is extensive phlegmon with multiloculated abscesses, extending from the left lower pharyngeal wall into the left lobe of the thyroid gland. Reactive lymphadenopathy in the left internal jugular lymph node chain is present.
Diagnosis: Infected 4th Branchial apparatus cyst
The main differential diagnostic considerations for a cystic neck mass in children include suppurative lymph nodes, abscess, thyroglossal duct cyst, lymphatic malformation, ranula, and branchial apparatus cyst. A branchial apparatus cyst (BAC) results from maldevelopment of an embryonic branchial apparatus (branchial cleft, arch, and pouch). Embryologically, 6 mesodermal branchial arches, separated by 5 external ectodermal branchial grooves (clefts) and 5 internal endodermal branchial pouches are present bilaterally. The majority of branchial apparatus anomalies are cysts that can arise from a remnant of a groove, arch, or pouch. A 2nd BAC is the most common and accounts for >90% all branchial cleft anomalies discovered in teens and adults. It represents 66%-75% of these anomalies discovered in children.
A 1st BAC is typically found as a cystic mass around the pinna or extending from external auditory canal (EAC) to the angle of the mandible. It can communicate with the external auditory canal. The 2nd BAC is typically found at or immediately caudal to the angle of the mandible, lateral to the carotid space and anteromedial to the sternocleidomastoid muscle. An associated fistulous track may extend from the cyst between the external & internal carotid arteries to the palatine tonsil. The cyst can extend to the carotid bifurcation, producing a beaked configuration, which has been called the "notch sign" and which is considered pathognomonic for a 2nd BAC. The 3rd BAC is typically found in the posterior cervical space behind the carotid sheath in the upper neck and along the anterior border of sternocleidomastoid muscle in the lower neck.
A 4th BAC is rare and seen more often in female infants. It can occur anywhere from the apex of pyriform sinus to the ipsilateral thyroid lobe. Involvement with the thyroid can be understood by noting that the thyroid gland arises from the 4th branchial arch. The most typical imaging finding of a non-infected 4th BAC is a unilocular thin-walled cyst found adjacent to or within the superior lateral aspect of the left thyroid lobe. Ninety-four percent of BACs involve the left side of the neck. These cysts normally show minimal or no peripheral contrast enhancement and no calcification. When infected, a thickened cyst wall is seen and often enhances with intravenous contrast media. Infected cysts often develop higher attenuation than noninfected cysts on CT images. Associated thyroiditis/thyroid abscess is not uncommon. An esophagram may demonstrate fistulous communication between the pyriform sinus and a 4th BAC, providing a pathway for spread of infection. Surgical resection of the cyst and its associated sinus or fistulous tract is necessary for complete cure. Medically treated or incompletely resected cysts/tracts are prone to recur.
Nessun commento:
Posta un commento