






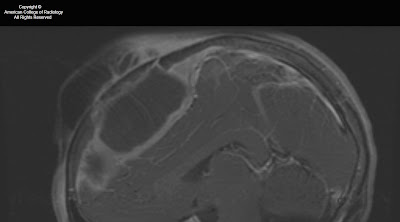
Findings
Figure 1: The image shows a large collection anterior to the frontal bone and a large epidural abscess with peripheral enhancement.
Figure 2: Erosion of the frontal bone. Sinus tract of the bone into the large anterior collection.
Figure 3: Large collection anterior to the frontal bone.
Figure 4: Large epidural abscess.
Figure 5: Large epidural abscess with peripheral enhancement.
Figure 6: Large collection anterior to the frontal bone. Large epidural abscess. Normal bone marrow signal. Abnormal bone marrow signal in the frontal bone.
Figure 7: Large collection anterior to the frontal bone with peripheral enhancement. Large epidural abscess with peripheral enhancement.
Figure 8: Abnormal bone marrow signal in the frontal bone. There is a lack of enhancement of the frontal bone. The abnormal dark bone marrow signal on T1 images and lack of enhancement on T1 post gad fat sat is consistent with dead necrotic bone from severe osteomyelitis.
Diagnosis: Pott's Puffy Tumor
Pott’s puffy tumor is a subperiosteal abscess of the frontal bone that appears as a localized swelling of the forehead associated with frontal osteomyelitis. Pott’s puffy tumor is a complication of frontal sinusitis or trauma, which is predominatly seen in the adolescent age group. However, there are a few case reports in adults. Pott’s puffy tumor is a rare complication of frontal sinusitis in the post antibiotic era but can be seen in patients with undiagnosed or partially treated sinusitis. Patients will typically present with frontal scalp swelling, headache, fever, nasal drainage, and frontal sinus tenderness. Ocassionally, Pott’s puffy tumor can mimic findings of preseptal or orbital cellulitis. In severe cases, there will be neurologic decompensation. Varying degrees of hemiparesis, obtundation, papillary dilatation or aphasia have been described in case reports.
Imaging is necessary to exclude intracranial complications such as epidural abscess. Pott’s puffy tumor can also be associated with dural sinus thrombosis, meningitis, subdural empyema, epidural abscess, brain abscess, and rarely seizure. Intracranial infection is caused by posterior extension from the frontal sinus while preseptal and orbital cellulitis is caused by downward spread from the frontal sinus to the orbit. Younger children who do not have pneumatized frontal sinuses, are more likely to have ethmoid sinusitis. Orbital cellulitis is a more common complication in patients with ethmoid sinusitis.
Patients must be treated with a combination of surgery and long-term antibiotic therapy.
Nessun commento:
Posta un commento